Why Vaginal Infections
Keep Coming Back
Recurrent vaginal infections such as bacterial vaginosis (BV), thrush (Candida), and urinary tract infections (UTIs) are often linked to vaginal microbiome imbalance.
Many women experience vaginal infections such as bacterial vaginosis (BV), thrush (Candida), or urinary tract infections (UTIs) more than once.
For some women, these infections keep returning again and again, sometimes for months or even years. If this has happened to you, you are not alone — and in many cases the underlying reason is vaginal microbiome imbalance, also known as vaginal dysbiosis.
Understanding why infections recur is the first step toward breaking the cycle.
Understanding Vaginal Dysbiosis
The vagina contains a complex community of bacteria known as the vaginal microbiome. In healthy vaginal environments, this ecosystem is usually dominated by Lactobacillus bacteria.
These protective bacteria help maintain: a healthy acidic vaginal pH, natural protection against harmful organisms, stability within the vaginal ecosystem
When Lactobacillus levels become depleted, the vaginal environment can become unstable.
This allows opportunistic organisms to grow,
such as: BV-associated bacteria, Candida species (thrush), bacteria associated with UTIs, mixed dysbiosis patterns. When this imbalance persists, women may experience recurrent infections rather than isolated episodes.
Why Standard Treatment Sometimes Fails
Many treatments focus on eliminating the infection itself. For example: Antibiotics for bacterial infections such as BV or UTIs, Antifungal medications for Candida (thrush). These treatments can be very effective at reducing the organisms causing symptoms.
However, if the underlying microbiome imbalance remains, the environment may still allow infections to recur. This is why some women experience a pattern
infection → treatment → temporary improvement
→ recurrence.
Addressing the underlying drivers of dysbiosis is oftennecessary to break this cycle.
Our Approach: Investigating the Underlying Causes
When infections are recurrent, our consultations focus on understanding why the vaginal
microbiome has become disrupted.
This begins with a thorough clinical history, which may include discussion of: symptom patterns and recurrence frequency, previous infections and treatments, antibiotic history, hormonal influences, contraceptive use, sexual health and partner factors, menstrual cycle patterns, menopause or perimenopause symptoms, medications and medical history, lifestyle factors that may affect microbiome health.
Understanding these factors helps identify patterns contributing to recurrent dysbiosis.
Vaginal Microbiome Testing/Mapping
For women experiencing persistent or recurrent symptoms, vaginal microbiome testing may be recommended.
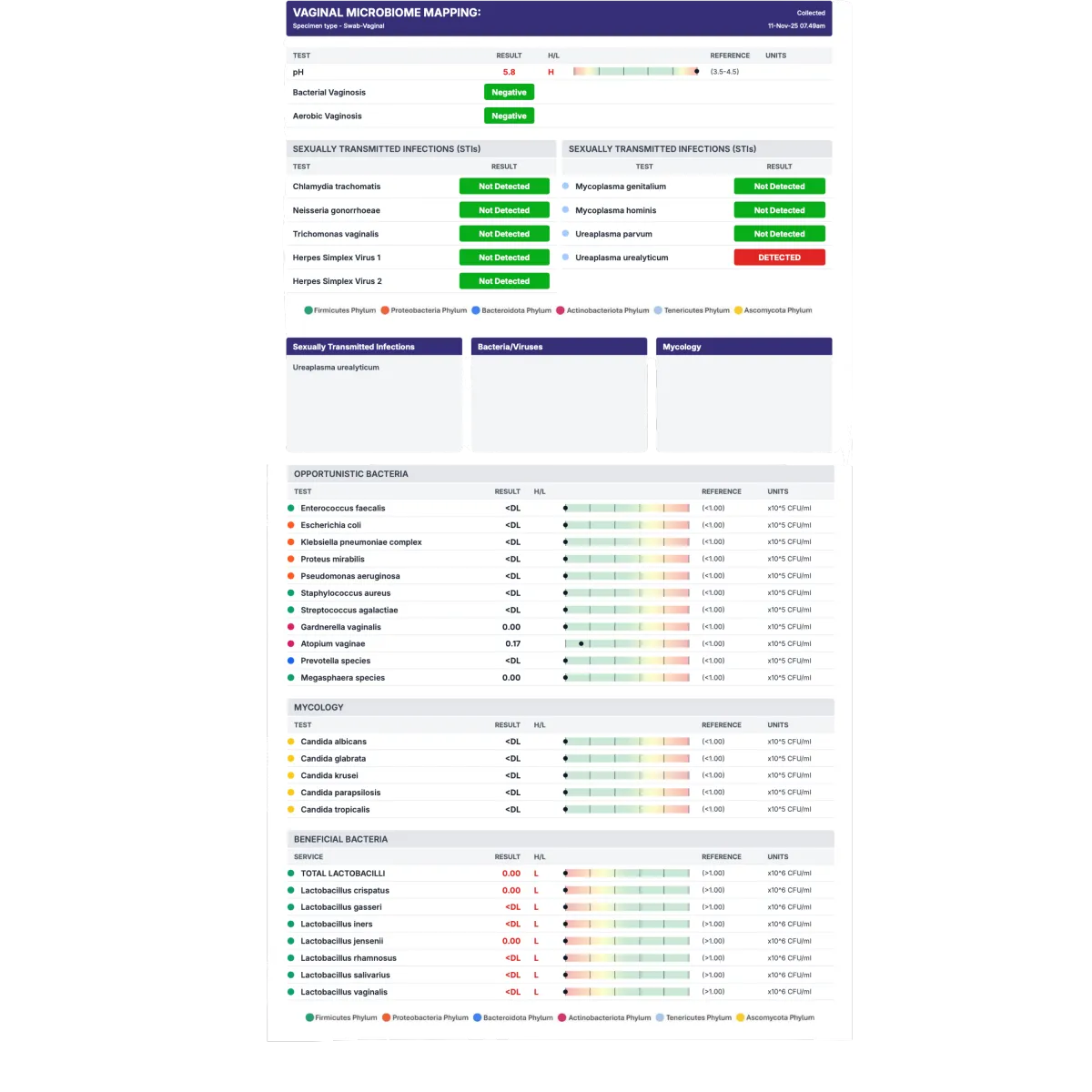
We commonly utilise Vaginal Microbiome testing, which provides detailed insight into the vaginal ecosystem.
This test may identify: levels of protective Lactobacillus species, presence of BV-associated bacteria, Candida species, including non-albicans Candida, bacterial species associated with dysbiosis, overall vaginal microbiome balance
This information helps guide more targeted treatment strategies, particularly in recurrent cases where standard treatments have
not provided lasting relief.
Treatment: Addressing Both Infection and Microbiome Balance
Management may involve several steps depending on the underlying findings.
Treating the Active Infection. If specific organisms are identified, conventional medical treatment may be recommended/commenced.
This may include: antibiotics for bacterial infections, antifungal medications for Candida infections, antiviral medications where appropriate, biofilm-disrupting strategies in some recurrent cases.
Where BV is recurrent, partner treatment may sometimes be recommended in line with current clinical guidance.
Restoring Vaginal Microbiome Balance
Once active infections are treated, attention is often directed toward restoring a healthy vaginal microbiome. This may include: targeted probiotic therapy to support Lactobacillus populations, strategies to restore vaginal pH balance, supporting long-term microbiome stability.
In some cases, we may also discuss: dietary factors that support beneficial bacteria, prebiotic foods that help nourish healthy microbial communities, lifestyle factors that influence vaginal health
The aim is to help restore microbial stability, reducing the likelihood of recurrence.
Breaking the Cycle of Recurring Infections
Recurrent vaginal infections can be frustrating and distressing, particularly when symptoms keep returning despite treatment.
By combining: careful clinical assessment, targeted conventional treatment, microbiome investigation, strategies to support long-term vaginal health.
It is often possible to break the cycle of recurring dysbiosis.
When to Seek Further Assessment
You may benefit from a more detailed assessment if you experience: BV that keeps returning, recurrent thrush infections, frequent UTIs, vaginal symptoms that return soon after treatment, persistent vaginal discomfort or discharge.
These symptoms may indicate an underlying vaginal microbiome imbalance that requires a more comprehensive approach.
Book a consultation if you would like to explore the underlying causes of recurrent vaginal infections and discuss personalised treatment options.
For enquiries feel free to get in touch.
We provide confidential, integrative women’s health care via telehealth — accessible, private, and designed for long-term results.
Email us: [email protected]
© Copyright 2026. Kylie Sayce NP. All rights reserved.
Terms and Conditions
