Case Study Recurrent “BV” That Wasn’t BV
Patient Background
A woman in her 40s presented with a ~3.5 year history of recurrent vaginal symptoms, including discharge, odour, irritation, and cyclical flares.
She had been repeatedly diagnosed with bacterial vaginosis (BV) and managed by multiple healthcare providers, including GPs and gynaecologists.
Previous management included: Multiple courses of oral antibiotics; Temporary symptom improvement followed by recurrence, Increasing frustration and impact on quality of life: Despite ongoing care, symptoms persisted often returning monthly.
Clinical Perspective
The frequency of recurrence and lack of sustained response raised concern that the underlying issue had not been fully identified.
Additional contributing factors included: Perimenopausal hormonal changes; Vaginal dryness suggesting a hypo-oestrogenic state; Delayed initiation of prescribed vaginal oestrogen; Repeated antibiotic exposure without microbiome restoration.
Given this pattern, vaginal microbiome testing was recommended to move beyond a symptom-based diagnosis and identify the true driver of recurrence.
Microbiome Testing Results
Results revealed a significantly different clinical picture: Bacterial vaginosis: Negative; Aerobic vaginitis: Positive; Streptococcus agalactiae (Group B Strep): Markedly elevated; Vaginal pH: Elevated (5.1); Candida species: Not detected; STIs: Not detected; Total Lactobacillus: Below detectable levels
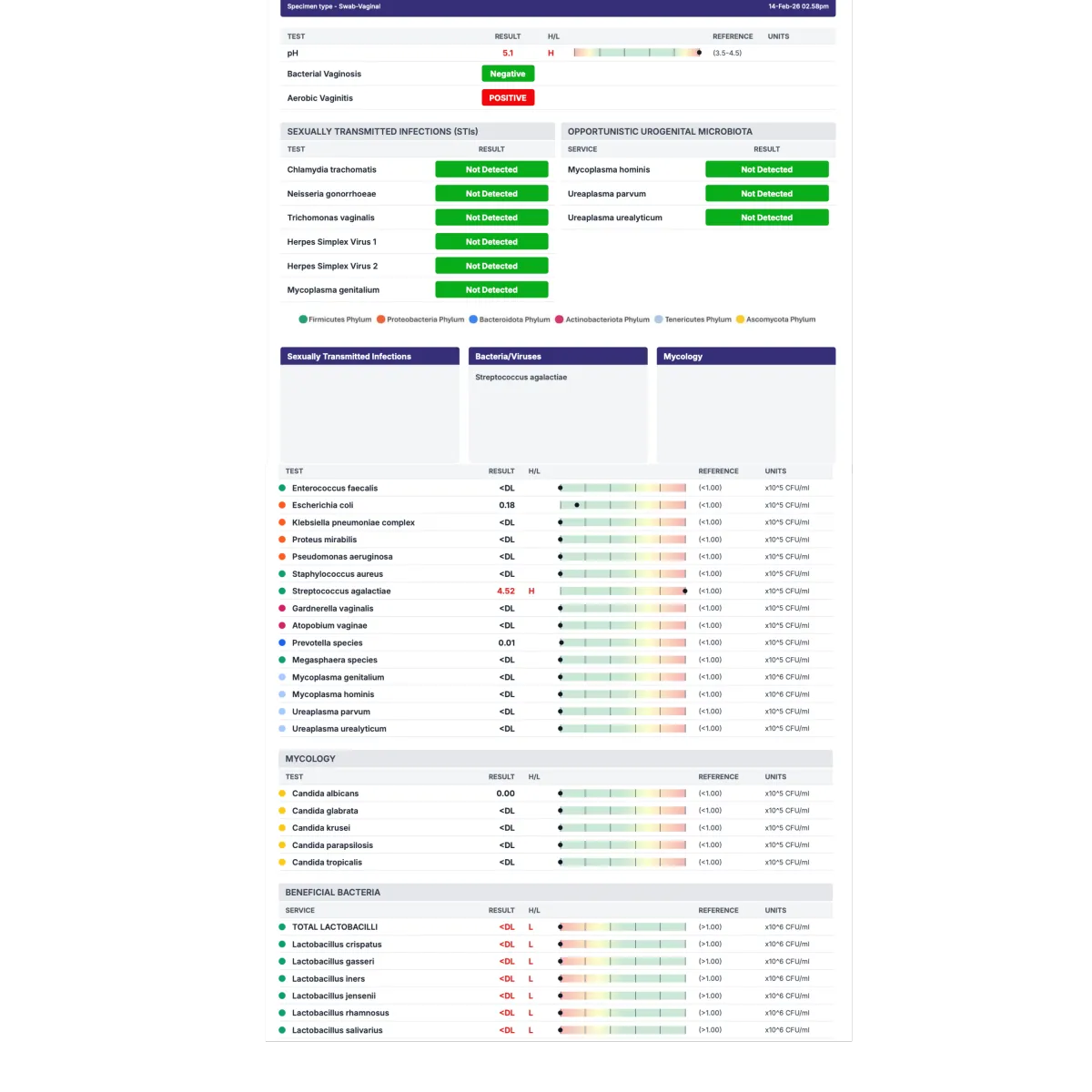
Clinical Interpretation
These findings confirmed that: The condition had been misclassified as recurrent BV; The primary issue was aerobic vaginitis, not BV.
There was complete depletion of protective Lactobacillus species, Elevated vaginal pH was allowing pathogenic bacteria to persist
Importantly, prior management had focused on suppressing bacteria rather than restoring the vaginal ecosystem.
Repeated antibiotic use likely: provided short-term symptom relief but further disrupted the microbiome by reducing already depleted Lactobacillus populations.
Additionally, a low oestrogen vaginal environment contributed to: Reduced epithelial integrity, Reduced glycogen availability, Impaired ability for Lactobacillus to re-establish
Treatment Approach
Management focused on both targeted antimicrobial therapy and restoration of the vaginal microbiome environment.
1. Targeted Antimicrobial Therapy - Antibiotic therapy for 7 days - Chosen to: Target aerobic organisms (including Group B Streptococcus)
Note: Due to a penicillin allergy, first-line antibiotic options were not appropriate, and an alternative targeted therapy was selected.
2. Microbiome Restoration Strategy: A. Vaginal Probiotic Therapy: Initiated after completion of antimicrobial treatment; Designed to reintroduce beneficial Lactobacillus species. B. Vaginal Oestrogen (Ovestin): Commenced twice weeklyTo: Restore vaginal tissue health, Increase glycogen availability, Support recolonisation of protective bacteria. C. Oral Probiotic Support - Continued as an adjunct. While not sufficient alone, this may support broader microbiome stability.
3. Supportive & Preventative Measures: Avoidance of vaginal irritants, Education around vaginal pH and microbiome balance, temporary barrier protection considerations during treatment phase.
Outcome
This case highlights a critical shift in approach: The issue was not persistent infection — it was persistent misdiagnosis.
By identifying the correct underlying condition: Treatment could be targeted appropriately, The vaginal environment could be actively restored, The cycle of recurrence could be interrupted at its root cause allowing decrease in symptoms and episodes of recurrence.
Key Insight
When Lactobacillus is depleted, the vaginal microbiome cannot self-regulate. In this state: Repeated antibiotic treatment alone is unlikely to provide lasting resolution; Restoration of the vaginal environment is essential for long-term outcomes
Clinical Takeaway: This case demonstrates the importance of: ✔ Moving beyond symptom-based diagnosis, ✔ Identifying the specific microbial drivers of symptoms, ✔ Addressing both infection and the underlying ecosystem
For enquiries feel free to get in touch.
We provide confidential, integrative women’s health care via telehealth — accessible, private, and designed for long-term results.
Email us: [email protected]
© Copyright 2026. Kylie Sayce NP. All rights reserved.
Terms and Conditions
